
Embracing the Call for Resilient Healthcare Design
By Richard Shiga and Jenny Cestnik, AIA, ACHA, EDAC, NCARB
When the novel influenza virus H1N1 began circulating across the globe in 2009, our healthcare clients—many of whose projects were in the late stages of design and construction—were confronted with a challenge that has similar echoes today.
While some were willing to implement measures like negative-pressure rooms, others wondered whether the investment was warranted. After all, severe pandemic outbreaks were thought to occur only once every hundred years.
The shift in sentiment these past 15 months, however, could not be starker. Clients unanimously recognize that pandemic-responsive facility design, planning, and mechanical systems are vital for building resilient healthcare systems. They also recognize that these infectious disease control measures will help reassure patients and families when they seek care, and help frontline staff and caregivers feel confident that they are looked after when they arrive for work.
For healthcare designers and planners at ZGF, this marked change has afforded us the opportunity to challenge long held assumptions, and in the process, imagine a far better patient and staff experience even beyond the pandemic setting.

The landscape outside the Seattle Children’s South Clinic in Federal Way, Washington, welcomes patients and families.
For those who are all too familiar with how aerosolized droplets travel indoors, spending less time in crowded indoor spaces could be a welcome change that puts patients at ease. For many healthcare systems, one of the first and most visible pandemic responses was to deploy outdoor triage tents. As we look for more long-term solutions, one of the biggest design opportunities is a re-think of the waiting room and check-in process.
One such solution is utilizing outdoor spaces to greet and queue patients. Visitors might arrive to a landscaped path with seating areas before being led to the entrance with “breadcrumbs” – a runnel of water, a distinctive sequence of plants, pavement treatments, or interpretive elements. Doing so enhances the arrival experience for everyone including those who cycle or take public transportation to their appointment or job. Beyond serving as circulation and an amenity, these landscapes can be calming and uplifting. Outdoor seating and fresh air also offer respite to caregivers and staff.
Those who wait for their appointments outside or opt to stay in their cars might appreciate remote updates via text or mobile app—the kind of technology experience they have likely already come to expect.
Separating Flows
Although U.S. hospitals have long designated entries for patients with more acute needs or who might be contagious, that hasn’t been the case for freestanding ambulatory clinics. Secondary entrances, perhaps typically used for staff, can be designed to be easily operated as a dedicated screening and triage area during future pandemics or flu seasons. Coupled with separate patient flows inside the facility, we can reduce the likelihood of potentially infectious patients comingling with others.
Staff Workspaces and Telehealth
The shift to open, team-based caregiver workspaces in recent years, meant to encourage closer collaboration between caregivers, also poses a challenge. Smaller desks often place providers and staff in closer proximity to one another.
Moving forward, employing creative furniture solutions—including wider and longer desks that provide greater separation between stations—can help maintain the physical distancing we’ve grown accustomed to during the pandemic. Partitions between stations can help limit the spread of airborne droplets, and also have the benefit of helping with acoustic concerns rampant in these larger collaborative spaces. Furniture solutions address the need for flexibility as staffing scales up and down without needing more-expensive architectural interventions.
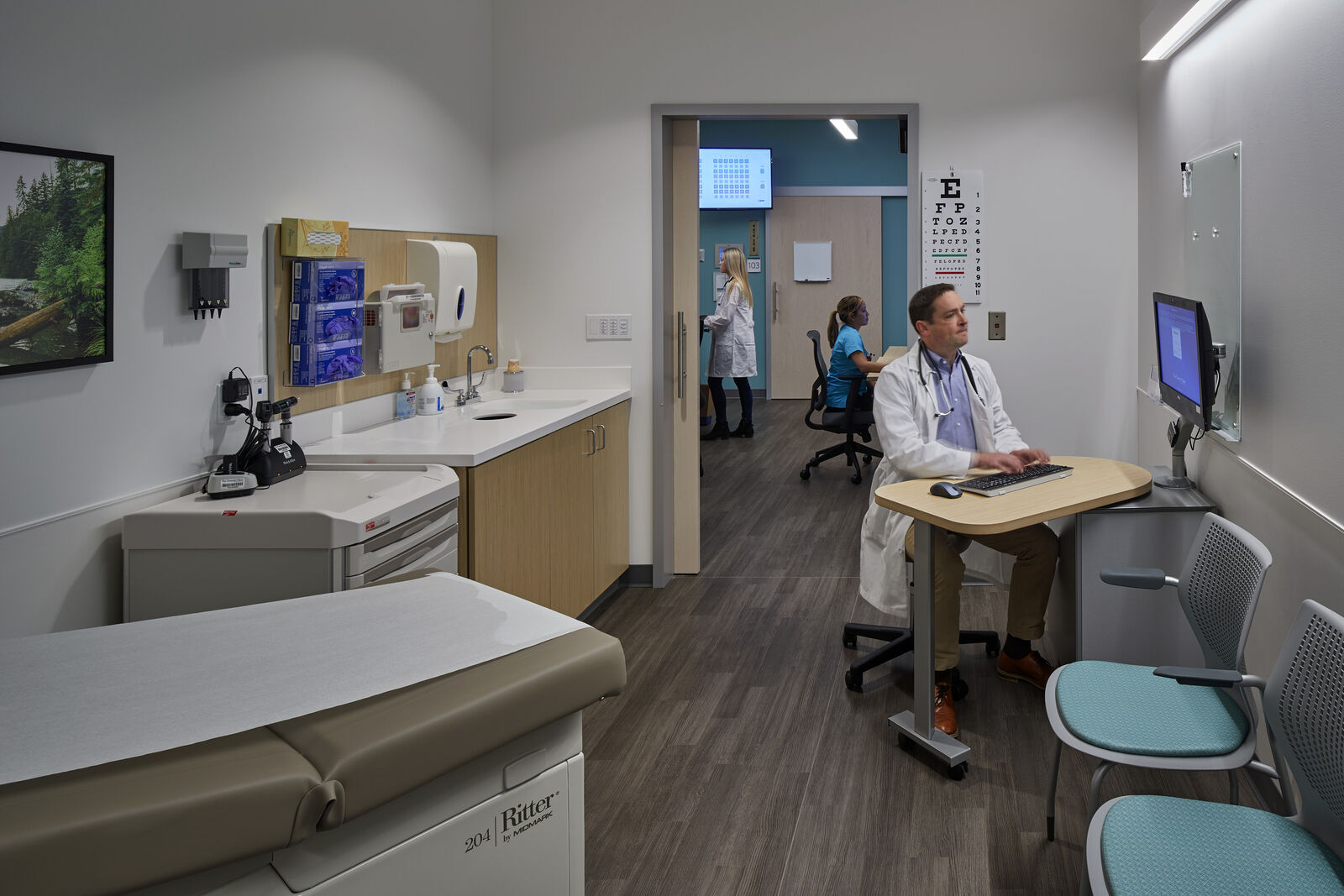
With the wide adoption of telehealth, a fraction of exam rooms—at least one in four—should also be telehealth-capable when provider staffing models include a mix of in-person and virtual visits. That means offering providers a touchdown space with appropriate lighting, acoustics and technology that meet patient-privacy standards.

A stairway at CHI St. Anthony Hospital, which serves the Pendleton, Oregon area.
Feature stairs have become a hallmark of healthcare design in order to promote active lifestyles and healthy habits. Coupled with integrated wayfinding solutions, they also support one-way circulation throughout a clinic. Dedicating “up” stairs and “down” stairs reduces the amount of path-crossing. Limited occupancy elevators remain available for those who need them, but require additional oversight.
Touchless Everything
High volumes of people stream in and out of clinics each day. Hands-free doors and elevators that open with the use of card readers are an obvious way to keep surfaces germ-free, but they also pose security challenges. The good news is that door manufactures are hard at work on potential fixes, like sensors to detect when cardholders and patients pass in and out of entryways before automatically closing.
Another vexing challenge is the issue of hand drying in restrooms. We know that automated dryers can be problematic. We also know that while paper towels are perhaps the least eco-friendly solution, they are the most hygienic (that is, until the next breakthrough in hand dryers).
If the current pandemic has taught us anything, it’s that the value of being prepared cannot be overstated. With some simple yet strategic design measures to make our facilities safer, more flexible and future-ready, healthcare systems will be much better equipped to care for patients, families and staff in the long run.
Richard Shiga is a healthcare architect and project manager who specializes in projects requiring complex and creative design solutions at a wide range of scales. Jenny Cestnik, AIA, ACHA, EDAC, NCARB, is a medical planner, designer, and architect who is inspired by buildings that heal. Both work out of ZGF’s Portland office.